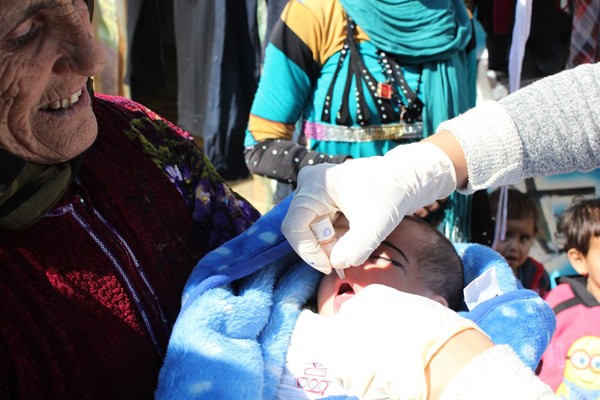
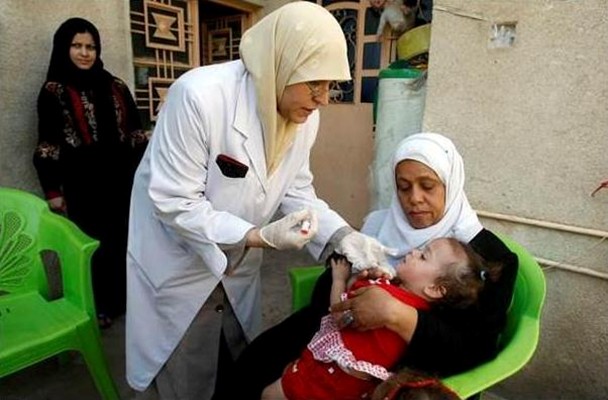
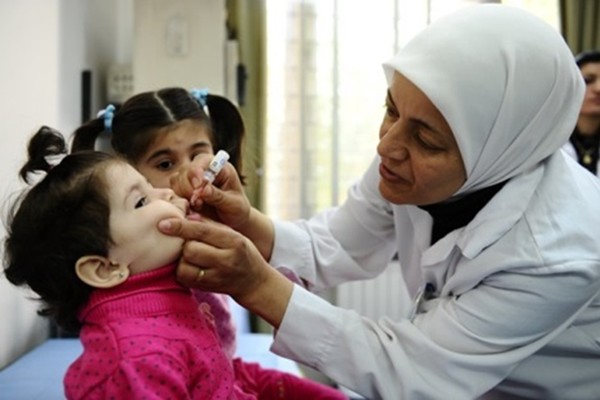
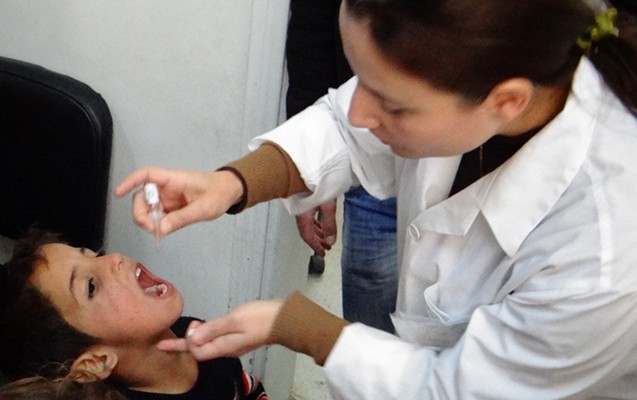
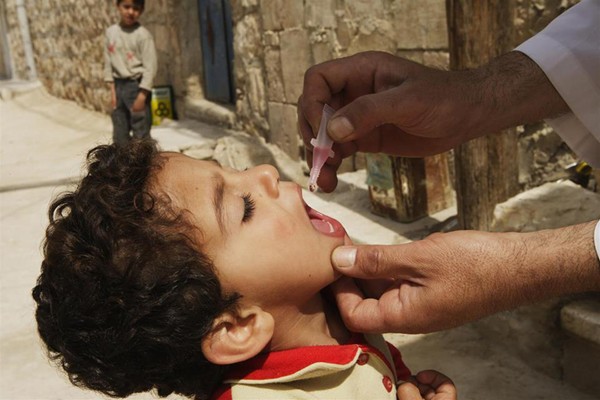
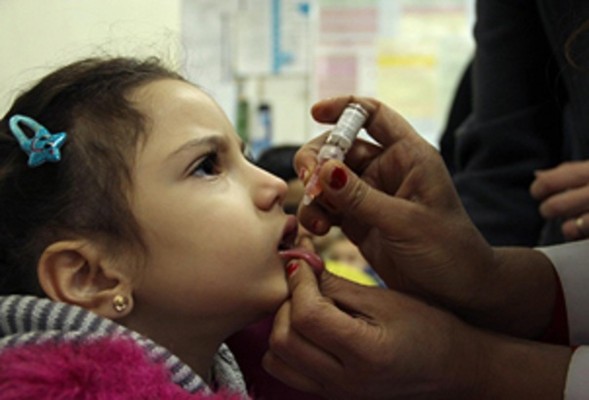
Dr Faten Kamel is on a flying visit to the WHO Eastern Mediterranean Regional Hub, stopping for meetings and to deliver a lecture on the relationship between polio and patients with primary immunodeficiencies. Then she’s off again – to Pakistan to take part in a polio programme management review.
Dr. Faten has travelled to every country in the Eastern Mediterranean Region, and many more besides. Alongside working as a Senior Global Expert for the programme, she is a wife, a mother, grandmother, and an informal mentor to women in public health.
Growing up in Alexandria, Egypt, Dr. Faten was exposed to the life-altering effects of polio on the people around her and was inspired by the work of her father, a surgeon and a Rotarian.
“My father was my role model, he had great passion for helping others and was also a Rotary Club president in 1989. His project for that year was on polio eradication.”
“Polio was prevalent in Egypt in those days. A number of people around me were affected. I was touched by their suffering in a place which was not highly equipped for people with special needs at that time.”

Making rapid gains against polio
After graduating from her Medical Degree and Doctorate in Public Health, and lecturing for several years at Alexandria University, Dr. Faten moved into a role for WHO. She found her niche working in the immunization team. “Immunization is the most cost effective public health tool – it can prevent severe and deadly diseases with just two drops or a simple injection – I strongly believe in preventive medicine,” she explains.
“I became the Eastern Mediterranean Regional Medical Officer for polio eradication in 1998. At that time many countries were still endemic.”
The 1990s and early 2000s were years of rapid gains against the virus. However to fully eradicate polio, it was becoming clear that the programme would have to be more ingenious than any disease elimination or eradication project that had come before.
Dr. Faten took a leading role. She explains, “Strategies for immunization and disease surveillance were established, and these methods evolved over time. We pushed the boundaries to make the programme more effective – shifting to house to house vaccination, detailed microplanning and mapping, retrieval of missed children and independent monitoring.”
“We started as a small team – covering different aspects of work and supporting all the countries. My team started the regular analysis and publishing of data in “Poliofax”, we supported the shift to case based and active surveillance and gradually added different supplementary activities including environmental surveillance.”
“I was blessed to have the support of my parents, my husband and my son. As a married woman I think it is very important to have the support of your family. I also had wonderful supervisors who believed in my capabilities and gave me opportunities. I am similarly impressed with many of the young women in the programme today.”

Overcoming outbreaks
Sometimes the biggest challenges for Dr. Faten and her team came out of the blue, such as when the programme faced huge polio outbreaks in areas that had become free of the virus.
“We didn’t expect polio to cause large outbreaks, but we were faced with them. To overcome the situation we started to work together as partners on effective response strategies within and across regions. The virus does not stop at borders and we had to coordinate multi-country activities.”
“In the polio eradication programme we cannot be satisfied with 80% or 90% coverage – we need to reach each and every child no matter where they are, even in the hard to reach and insecure places. So there was always a lot of innovation and adaptive strategies, we were thinking how can we bridge this, and reach these children.”
“That’s how we came up with access analysis and negotiation, days of tranquility, using windows of opportunities and short interval campaigns, community involvement and collaboration with NGOs, intensifying work at exit points, thinking out of the box all the time.”

Tracking polio down unexpected paths
Dr. Faten was determined to possess firsthand information on polio cases, no matter where they occurred. Sometimes, this led her down unexpected paths – such as when she travelled 21 hours through the Sudanese bush to track down a polio case in a remote village.
“I’ll never forget when a wild poliovirus type 3 (WPV3) case appeared in a very faraway place in Sudan after years without WPV3. I said, “I have to see it myself”. This mission was one of my most challenging fieldtrips.”
“We faced many difficulties, it was the rainy season, the car slipped on its side on our way and we arrived after midnight.”
“I thought the virus must have been hiding in this place for years. But I found the disease surveillance to be very good. Then by investigating, we found there was a wedding, and relatives were coming from another province, so I could nearly point my finger to where the virus came from. The virus was detected in that area and we managed to curtail its spread.

A career spent getting ahead of the virus
In 2016, Dr. Faten set up the Rapid Response Unit in Pakistan – a dedicated ‘A team’ that can jump into an at-risk area to mitigate virus spread. Today, she is working with medical professionals to ensure that individuals with primary immunodeficiencies get tested for poliovirus, as some of them are at risk of prolonged virus shedding.
What keeps her awake at night?
“I care about where we are not reaching. Polio eradication is beyond health – it needs all the sectors to come together especially in a big country. In the last strongholds of the virus we have population movement across the border, some areas that are difficult to reach, and there are some misconceptions.”
“If someone comes and says this area is inaccessible, this is not an answer for me. I ask: What should we do to reach? I like to make use of the ideas and experience that come from local people. The virus strongholds are in certain areas, so let us work closely with the people in these areas, empower them, and allow them to change the situation.”
Dr Faten is proud to be part of the polio eradication programme and looks forward to the day when polio eradication is achieved, so she can spend more time with her family in Australia.
“As a grandmother, I am especially determined to finish the job. I want my grandkids to grow up in a world free of polio. This will be my contribution to their futures.”