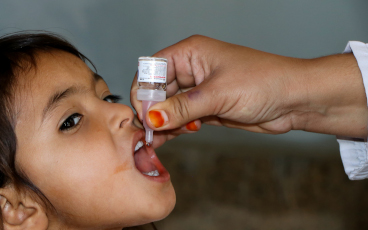
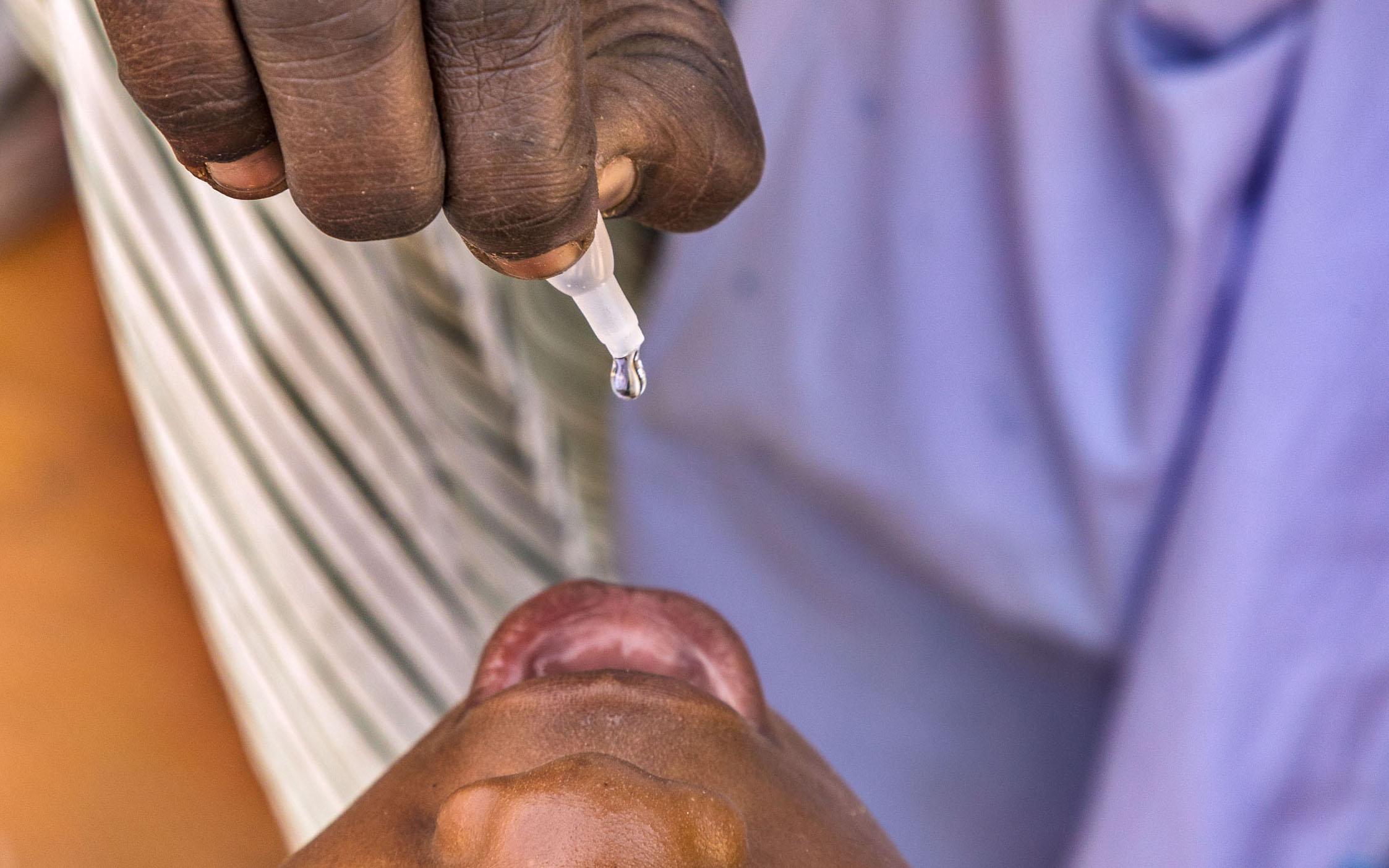
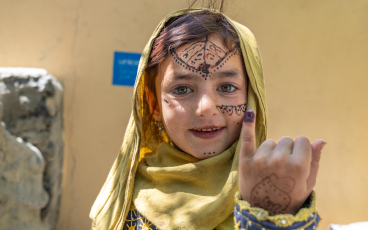Could this little girl become Africa’s last case of polio?
Polio has not been detected for a year, but that doesn't mean it’s gone
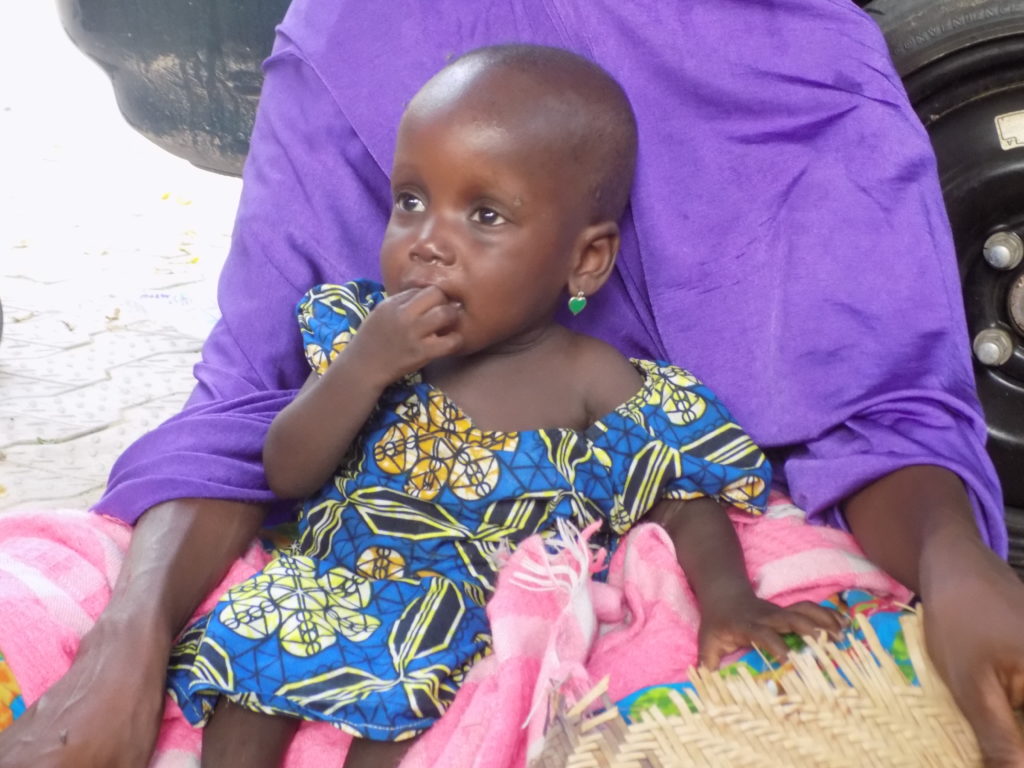
The photo shows a little girl in a blue dress, resting against her mother’s shawl, a tiny green heart hanging from her ear.
It is just over 12 months since two-year-old Yafanna Mamma became Nigeria’s most recently-reported case of wild poliovirus. But this anniversary provides little cause for cheer – last year, Nigeria was about to celebrate two years without any cases, only for four infants to arrive from deep inside conflict-affected territory, in the remote north-eastern state of Borno, paralyzed by polio. Yafanna was the last of them, arriving in the northern Nigerian outpost of Monguno malnourished and sickly.
The discovery of polio in these children underlines the challenges facing the polio eradication programme – and many other health and development initiatives – working in conflict zones. Amidst the ongoing humanitarian crisis in North-Eastern Nigeria, at least 200,000 children are estimated to still live in inaccessible areas, where insecurity is a constant threat. All humanitarian activity, including vaccination campaigns and disease surveillance, is made all the more difficult across these areas, and there is a significant risk that poliovirus continues to hide undetected, spreading among unvaccinated children in the area.
Yafanna’s paralysis was a lesson that when vaccination and disease surveillance efforts pose such a challenge, finding no polio cases does not mean that there is no virus.
Yafanna’s family – father Ali, mother Yagamallam and their two surviving sons – are a living example of the consequences of conflict on the health of families. Their small village, Zanari, is four hours’ walk into inaccessible territory north-east of Monguno, with no health centre and irregular access to vaccination campaigns.
“Since 2014, there is no health facility,” Ali says softly, seated beside his wife in the WHO-UNICEF joint office in Borno’s capital, Maiduguri. “The closest facility is in Monguno town and walking it takes many hours.”
They made that walk, carrying their infant daughter, two weeks after she had fallen sick with a high fever and they soon noticed she could no longer stand. When they arrived in Mongonu a worried doctor quickly referred them to Maiduguri, where they attended a health facility in a camp for internally displaced people.
“At the health facility they asked us to bring stool samples from our daughter, they gave us medicine, and after we went back home. The fever got better, but she stayed paralyzed.”
After two weeks, the military arrived, guarding a medical team which confirmed that little Yafanna, who had never received any doses of oral polio vaccine, had been found by the poliovirus.
“We had heard of this disease,” Ali says, looking down at the table. “But we didn’t know what it could do. Before the insurgency, vaccinators would visit us with a motorcycle. But after the insurgents came the vaccination teams stopped coming.”
The polio eradication programme is working hard in Nigeria to reach every child with the vaccine, and to find the virus wherever it is hiding. Vaccinators are steadily reaching more children, using strategies such as engaging and collaborating with local communities, vaccinating in camps for internally displaced people, and in different locations like markets and transit points. But there is still much work to do.
Little Yafanna never walked again. Three short months later after her paralysis, she contracted another disease – possibly whooping cough – and on 27 December 2016 after three days of coughing and fever, she died.
Ali now has been engaged to talk with the community about the threat of polio, and the importance of vaccination. “I pray that we can honour her life by making her the last polio case in all of Africa. So that her name is remembered. So that her life is remembered.”