From a small prefabricated container where the walls host detailed maps and desks prop up computer screens beaming data, tables and graphics, the Rapid Response Team at the World Health Organization’s (WHO) Regional Office for Africa coordinate polio outbreak response. The team work across the continent, where 12 countries are battling the vaccine-derived strain of the virus.
Dr Ndoutabe Modjirom, a former Chadian university professor-turned WHO medical officer, coordinates the multi-agency team, which was formed in September 2019. It is composed of twenty experts in operations and vaccination management, epidemiology, logistics, and communications. They are drawn from the core partners of the Global Polio Eradication Initiative (GPEI): WHO, the United Nations Children’s Fund (UNICEF), Rotary International, the US Centers for Disease Control and Prevention, the Bill & Melinda Gates Foundation, and Gavi, The Vaccine Alliance.
The team is mobilized whenever a new polio outbreak is confirmed in the African region.
The first 72 hours
“Our work starts once the lab confirms that a sample collected from either the environment or a paralysed child is caused by a poliovirus. Every minute that passes after the lab confirmation means that the poliovirus is circulating and risks infecting more children,” says Dr Modjirom.
Within the first 72 hours, the Rapid Response Team deploys Team A. This team includes the GPEI Coordinator alongside an epidemiologist, an operations officer, a vaccine manager and a communicator for development. The team works closely with the health authorities in the affected country along with the relevant WHO and UNICEF country offices to prepare a risk assessment and outbreak response plan. The emergency response vaccination campaign, called ‘Round Zero’, starts within 14 days.
Team B takes over from Team A after the first eight weeks and continues the outbreak response activities.
According to standard operating procedures for responding to outbreaks, the polio programme must implement three rounds of high-quality vaccination campaigns in response to every outbreak. Parallel to vaccination, countries must intensify disease surveillance activities to detect new cases of acute flaccid paralysis, a clinical symptom of poliomyelitis.
“Priorities are constantly shifting for the Rapid Response Team,” says Dr Christopher Kamugisha, who has been working with WHO since 1998. He has been a member of the Rapid Response Team since its inception and like the rest of the team has been chasing new polio outbreaks across the region.
“In August I was in Somali Region in Ethiopia supporting the outbreak response, conducting the first vaccination campaign round. On the second day of the campaign, Dr Ndoutabe informed me that a new case was detected in Cheporoni in Ghana and asked me to go and provide technical support,” Dr Kamugisha recalls.

Within 24 hours, he was on a plane to Accra through Addis.
“I arrived at noon the next day and went straight to support the national technical team in their preparations and risk assessment. I assisted with ensuring that their plans are in line with the international standard operating procedures set by the GPEI,” Dr Kamugisha says.
No cure for polio
Polio is a viral disease, multiplying in the intestines and transmitted from person to person mainly through a faecal-oral route or, less frequently, through contaminated water or food.
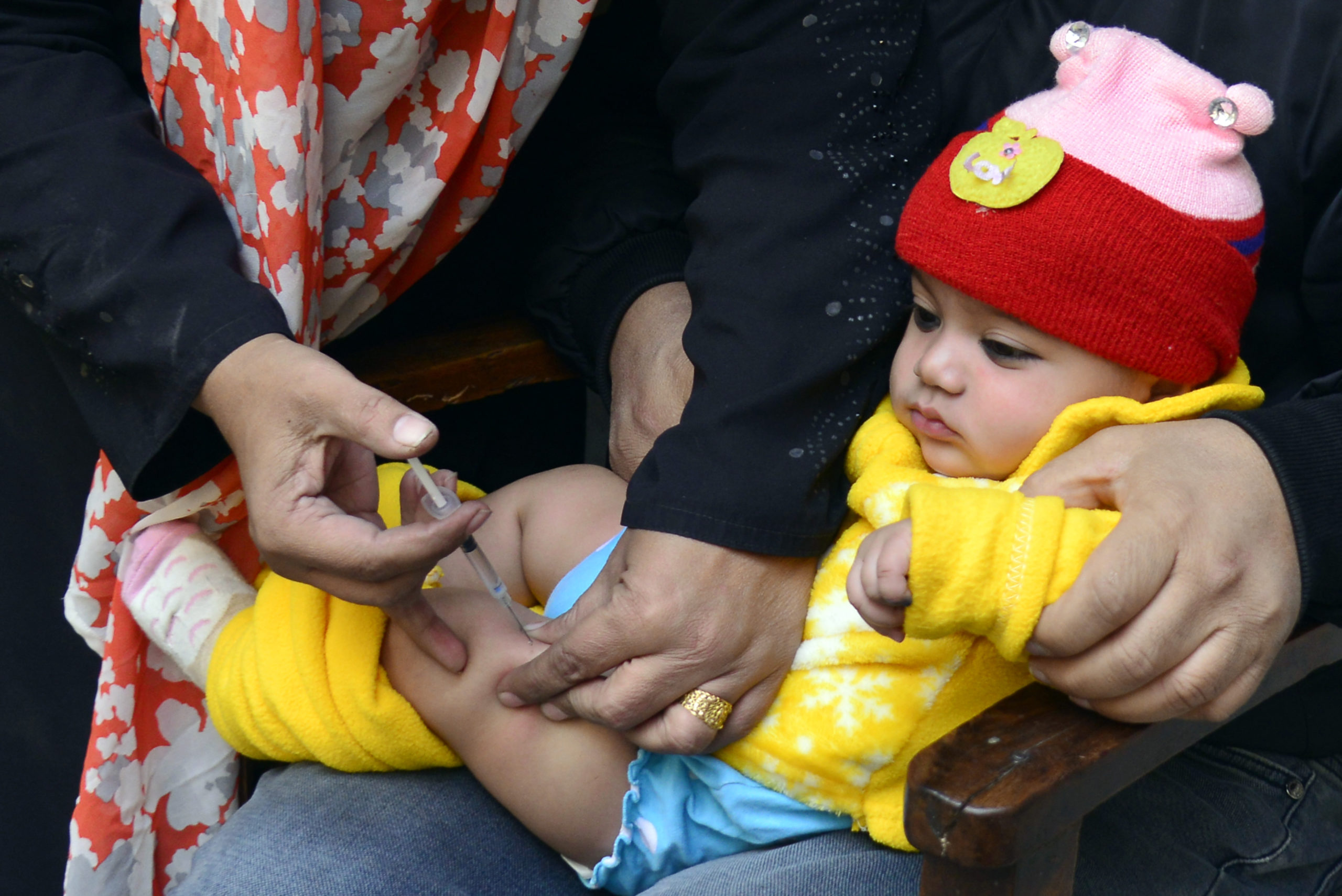
While there is no cure for polio, the disease can be prevented through administration of a simple and effective vaccine. That is why efforts are underway across the country to rapidly boost immunity levels in children and protect them from polio paralysis.
Thanks to the efforts of the GPEI and country governments, no wild poliovirus has been detected anywhere in Africa since 2016. This stands in stark contrast to 1996, a year when wild poliovirus paralysed more than 75,000 children across every country on the continent.
In 2020, the central challenge for the African Region is overcoming outbreaks of circulating vaccine derived poliovirus. Vaccine-derived polioviruses are rare, but can affect unimmunized and under-immunized populations living in areas with inadequate sanitation and low levels of polio immunization.
Countries experiencing outbreaks of vaccine-derived poliovirus in Africa are Angola, Benin, Cameroon, Central African Republic, Chad, Côte d’Ivoire, Democratic Republic of the Congo, Ethiopia, Ghana, Nigeria, Togo and Zambia. Reasons these outbreaks have occurred include weak routine vaccination systems, vaccine hesitancy, difficulty accessing some locations and low-quality vaccination campaigns, which have made immunization of all children challenging.
In addition to the response activities, the Rapid Response Team work to build the capacity of health workers and decision makers in countries that are not experiencing polio outbreaks, training them to be ready to respond if virus is ever detected.
The team also aims to recruit more women with expertise in outbreak response. Achieving gender balance amongst personnel through a more equitable recruitment process forms part of the GPEI Gender Equality Strategy 2019 – 2023, which was launched in May 2019.
By supporting countries during outbreaks, and building health system resilience in vulnerable settings, the polio programme is working to establish a sustainable legacy that will improve health long after global eradication of the virus.