Reposted with permission from Rotary.org

From the epidemics in the 1950s to the 1000 cases per day in the 1980s, polio’s devastation has seeped across generations. That is, until Global Polio Eradication Initiative and anchoring partners, Rotary International, WHO, UNICEF, CDC, and most recently, the Bill & Melinda Gates Foundation, united efforts and resources to develop a comprehensive polio eradication infrastructure.
Ranging from cutting edge research to dedicated laboratories to community engagement to sewage sampling, the polio infrastructure is as widespread as it is comprehensive. With presence in over 200 countries, the polio programme is second to none, making it one of the largest public-private health partnerships in history.
While the polio eradication infrastructure helps get us closer to a polio-free world, did you know that it is also used to fight and protect against other diseases, too? Here are five examples of the polio infrastructure at work:
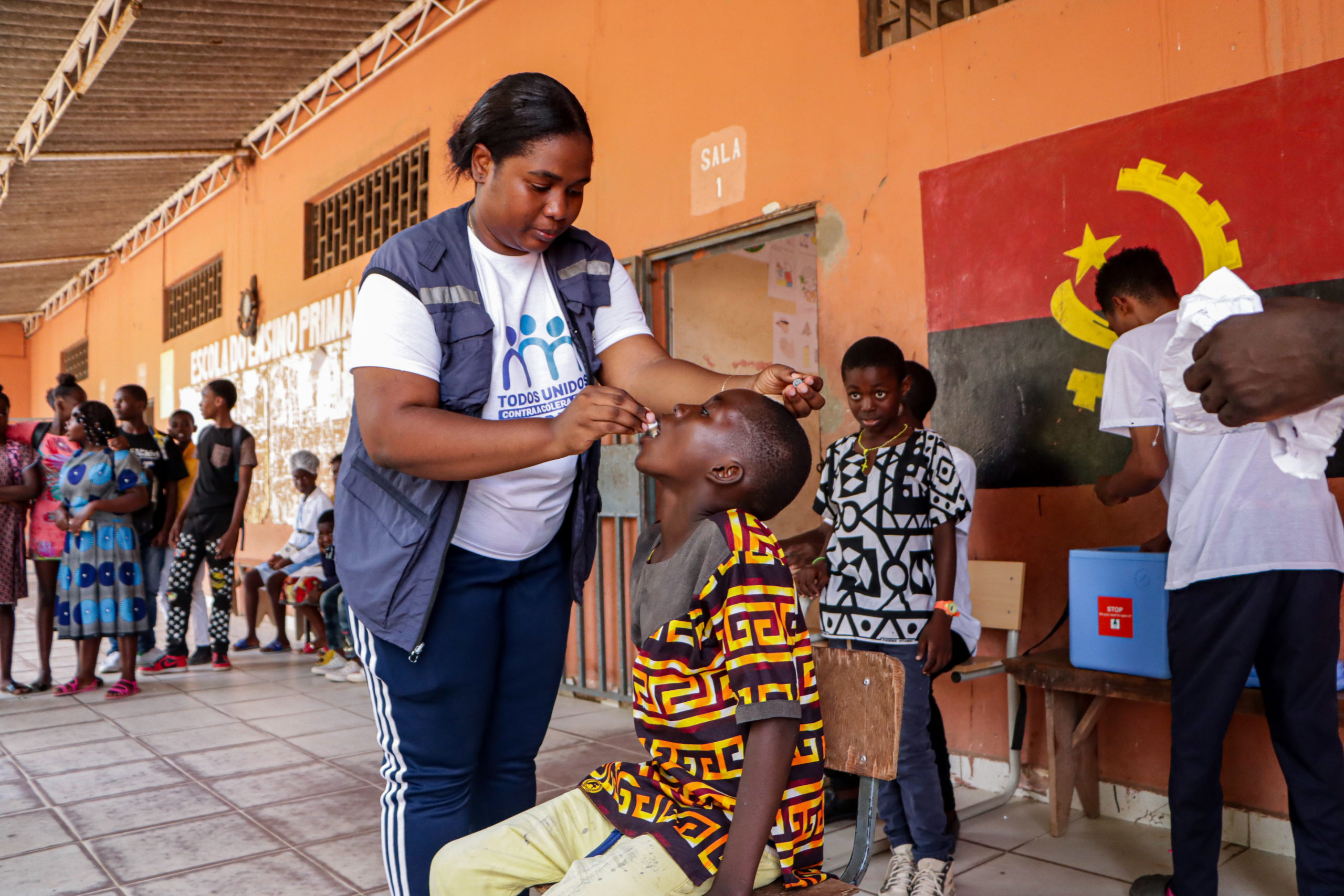
The cold chain
The Oral Polio Vaccine (OPV) requires constant refrigeration and vaccine must be kept cool between 2-8 degrees, or it risks losing its effectiveness. This is no easy task in countries and areas where electricity is either unavailable or unreliable.
So, the programme developed what is known as a cold chain system — made up of freezers, refrigerators, and cold boxes — to allow polio workers to store the vaccine and transport it over long distances in extremely hot weather. In Pakistan, a measles immunization program now relies on the same system. With the help of the cold chain, Sindh province recently reached its goal of immunizing more than 7.3 million children against measles.
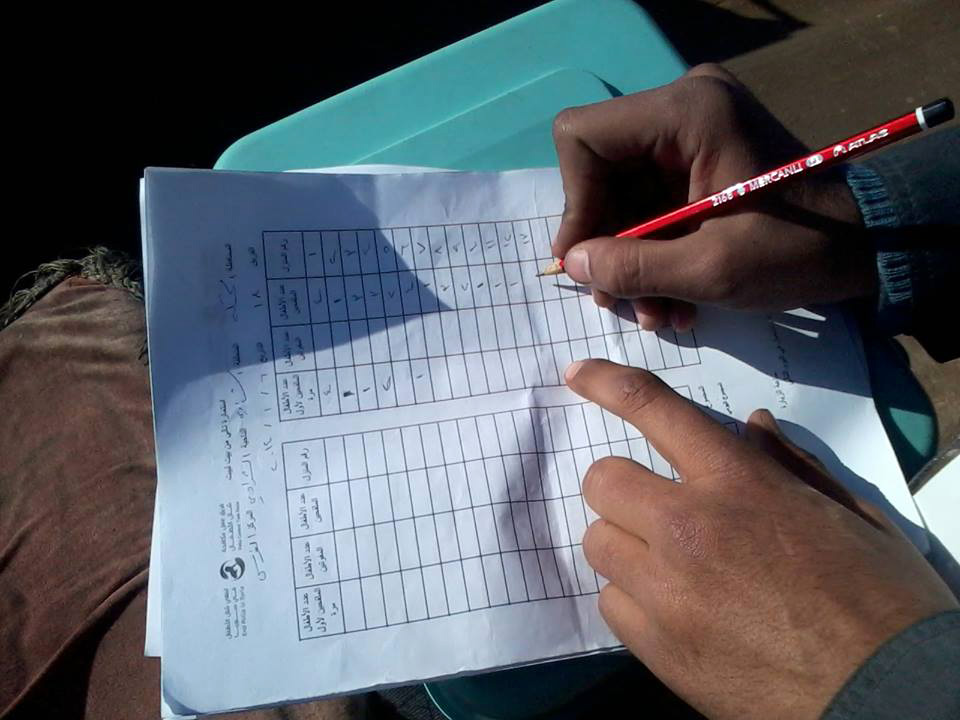

Microplanning
A critical component in immunizing more children against polio, especially in remote regions, is microplanning. A microplan allows health workers to identify priority communities, address potential barriers, and develop a plan for a successful immunization campaigns.
The workers collect as many details as possible to help them reach and vaccinate all the children. This strategy has helped keep India polio-free for five years. Now the Mewat district of India is using microplanning to increase its rates of vaccination against measles and rubella.
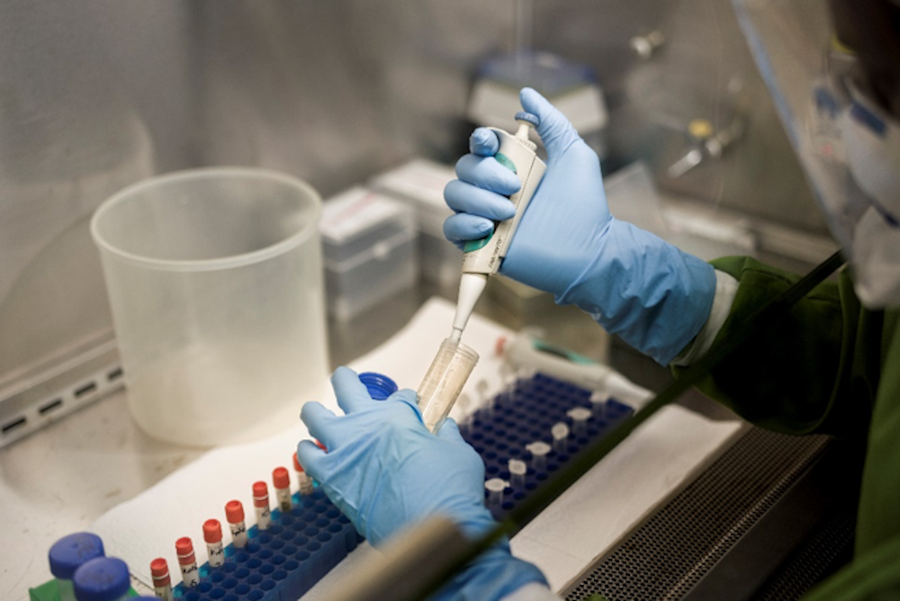
Surveillance
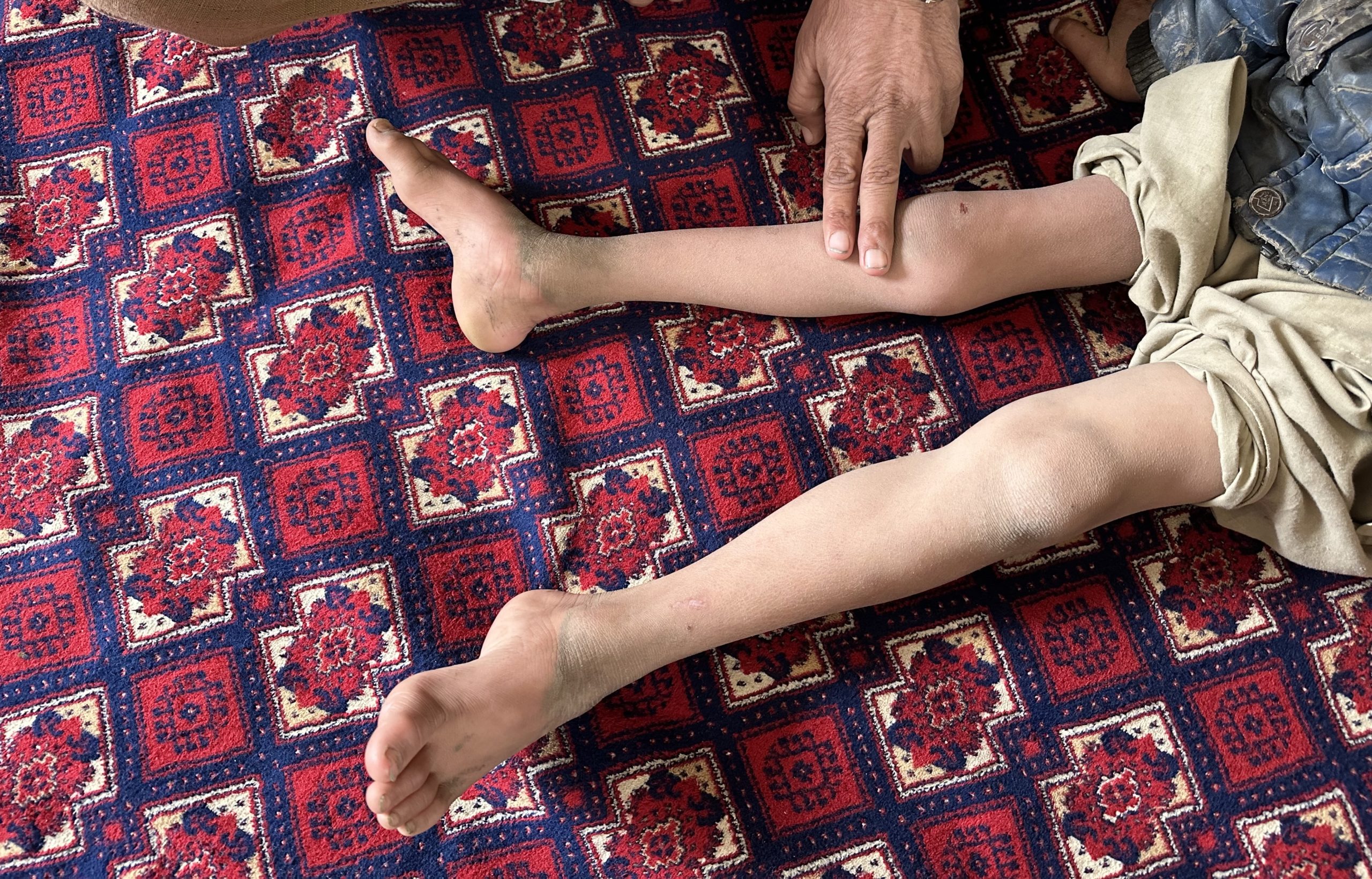
The polio surveillance system helps detect new cases of polio and determines where and how these cases originated. Environmental surveillance, which involves testing sewage or other environmental samples for the presence of poliovirus, helps workers confirm polio cases in the absence of symptoms like acute flaccid paralysis (AFP).
In Borno state in Nigeria, the AFP surveillance system is now being used to find people with symptoms of yellow fever and was one of many tactics used during a 2018 yellow fever outbreak that resulted in the vaccination of 8 million people.
Contact tracing
Since polio is a transmittable disease, health workers use contact tracing to learn who has come in contact with people who might be infected. Contact tracing was also critical to containing an Ebola outbreak in Nigeria in 2014. When a traveller from Liberia was diagnosed with Ebola, Nigerian officials were able to quickly trace and isolate the traveller’s contacts, helping prevent the disease from spreading further.

Emergency operations centres
An important part of the polio infrastructure that Rotary and its partners have built is the emergency operations centres network. These centres provide a centralized location where health workers and government officials can work collaboratively and generate a faster, more effective emergency response. The emergency operations centre in Lagos, Nigeria, which was originally set up to address polio, was adapted to handle Ebola, and it ultimately helped the country respond quickly to an Ebola outbreak. Only 19 Ebola cases were reported, and the country was declared Ebola-free within three months.