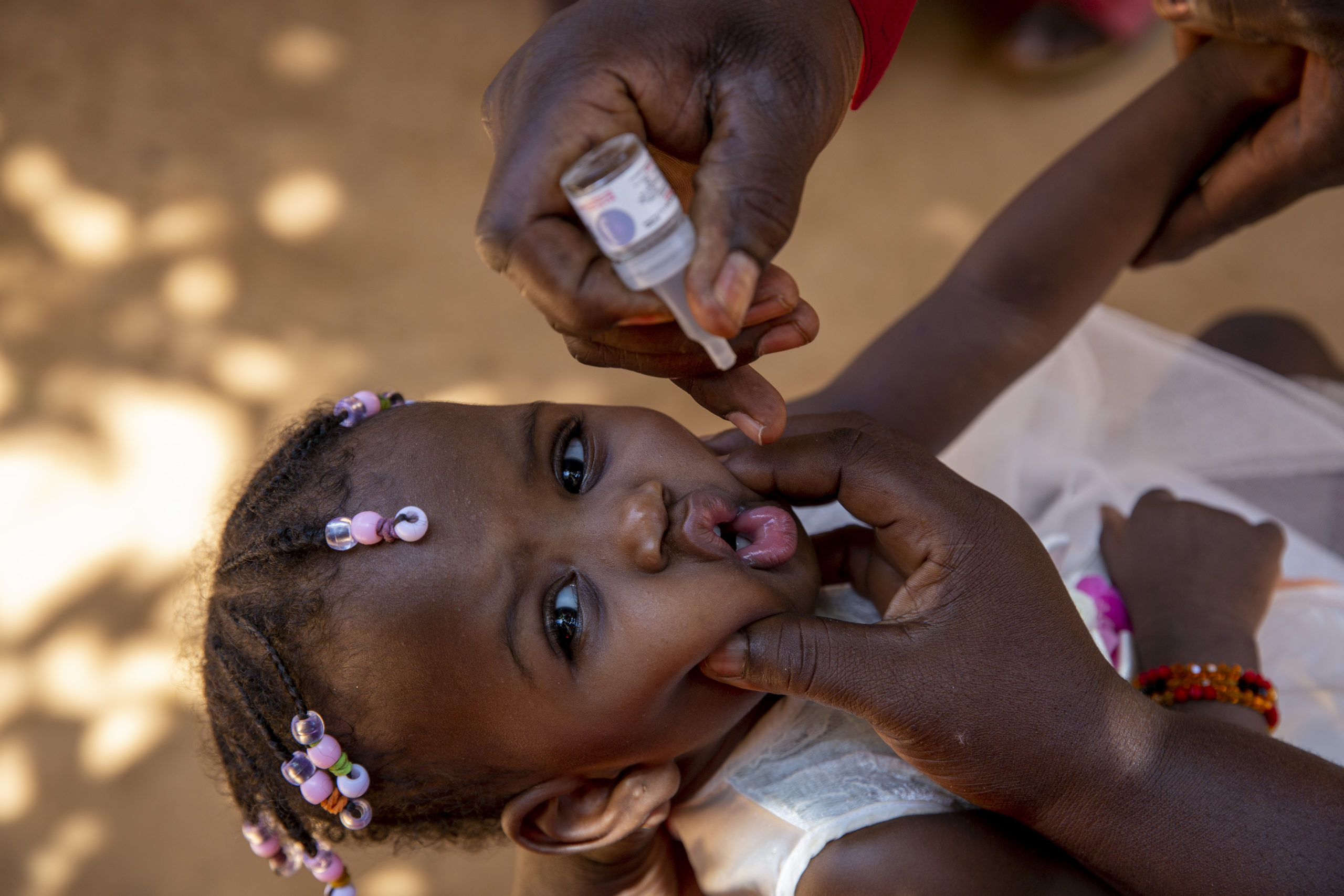
WHO/L.Dore
It has been 18 months since Nigeria, once considered one of the biggest challenges to global polio eradication, saw a child paralysed by wild poliovirus. Yet this tremendous achievement, tribute to the hard work of many across the country, is not the end of the road for Nigeria’s polio programme. Now is the time to build resilience against the virus; and also to seize the opportunity to plan for how the polio infrastructure can make a sustainable difference to the health of some of the most vulnerable communities long into the future.
This year, countries with strong polio programmes, including Nigeria, are planning for how to transition the expertise of their human and technical infrastructures to other health programmes, once a polio-free world has become a reality.
“Becoming polio-free gives such a boost of confidence to countries,” explains Dr Hamid Jafari, former Director of the Global Polio Eradication Initiative. “Success in public health breeds more success; this is happening in Nigeria right now.”
In February, Ministers of Health from across Africa will gather at the first Ministerial Conference on Immunization to find solutions to the challenges facing their routine immunization systems. The polio programmes in countries like Nigeria have important lessons to offer routine immunization across the region; from ensuring equitable access to vaccines and engaging communities even in the most remote places, to the role of political leadership and accountability in protecting children against vaccine-preventable diseases.
Political leadership

In 2012, 122 children were paralysed by polio in Nigeria. The tide changed when the Government of Nigeria took ownership of the programme, setting up the National Polio Emergency Operations Centre to bring together the expertise of partners, ensure accountability and coordination, and to introduce data-driven, innovative solutions. The impact of this spread far beyond polio, strengthening routine immunization and even helping to coordinate the emergency responses to the Ebola outbreak in 2014 and the current Lassa fever outbreak.
“Becoming polio-free gives such a boost of confidence to countries,” explains Dr Hamid Jafari, former Director of the Global Polio Eradication Initiative. “Success in public health breeds more success; this is happening in Nigeria right now. Everyone at all levels becomes more willing to take on huge challenges because they are riding on momentum of polio eradication.”
Boosting routine immunization coverage
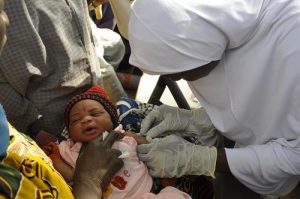
The polio programme in Nigeria has long worked hand-in-hand with routine immunization, but with low routine immunization coverage in the past, campaigns were necessary to boost immunity to a level that would stop transmission. Yet as the polio programme increased in strength, the relationship between the two meant lessons – on building community support, strengthening logistics and accountability and using data to inform action – had a roll-on impact. Between 2012 and 2015 in Kano, the number of children reached with all necessary doses of the oral polio vaccine increased from 61% to 94%; and the number of children reached with the full set of doses the pentavalent vaccine rose from just 41% to 91%.
The people who make things happen

The surge in polio capacity resulting from increased government commitment has brought over 12,000 volunteer community mobilisers (VCMs) and field volunteers to engage and inform communities on the importance of polio by visiting every home. Most often women with trusted positions in their villages, such as teachers and traditional birth attendants, VCMs are able to provide mothers with important information that goes beyond polio, such as the importance of routine vaccines, nutrition and hand-washing. Religious leaders engaged through the polio programme played an important role in addressing vaccine hesitancy in the country, and their influence is now helping to encourage families to get their children vaccinated against other diseases, alongside polio.

Going the extra mile
The Hard-to-Reach project is operational in 10 high-risk states in Nigeria. In Kano state alone, the project brings vaccines against polio and other preventable diseases to 432 remote settlements in Kano that house-to-house polio teams were struggling to access. The camps are built on the polio infrastructure but offer other services such as antenatal care, routine vaccines, basic medicines, screening for malnutrition and health education, which are desperately needed by families with no other access to healthcare.
A unique opportunity
Now is the time to plan for the future of projects like this, where the lessons learned and capacity built over the last three decades through polio eradication are playing an important role in other programmes. Governments have the opportunity to work with civil society, the health sector and donors to integrate polio funded infrastructure into ongoing public health programmes, so that the investments made in polio eradication continue to have an impact long into the future.
“It would be a very sad story if health camps like these were to stop,” said Dr Muhammad Sani Umar, the focal point for routine immunization for WHO in Kano. “However, we are discussing with the state on the sustainability of these projects to develop a plan together. My vision is for us to use the polio infrastructure to strengthen routine immunization, ensuring a better life for our children.”
“It will take a lot of work to sustain the progress we have made against polio in Nigeria, needing quality campaigns and surveillance, and also the improvement of routine immunization,” explained Dr Ado Mohammed, the Executive Director of the National Primary Health Care Development Agency for Nigeria.
As we near global polio eradication, the public health community has a chance to make the most of the experience, lessons, structures and people from the programme who are already doing so much for the health of children in countries across Africa.
Related